Services
During your initial consultation with Dr Ehlers he will perform a thorough examination and identify any associated problems you may have. This will help him to develop a treatment plan that specifically suits your problem/s and he will explain what is required to achieve a high quality result. He will also explain the risks of the various surgical procedures and answer any questions you may have. He will then, with your permission, inform your referring doctor and any other health care providers who you elect to include, about your diagnosis and proposed treatment plan. 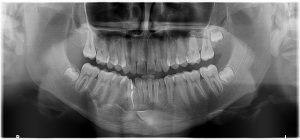 Removal of impacted teeth Surgical removal of all wisdom teeth and impacted teeth. An impacted tooth is a tooth that is unable to erupt into its normal position in the jaw. This is usually caused by the tooth becoming blocked in-between two adjacent teeth or by the tooth being formed in an abnormal position. The most commonly affected teeth are the wisdom teeth/third molars and the canines. Wisdom teeth are the last teeth to erupt in your mouth, usually between the ages of 17 and 25. In ancient times, the rough diet people followed resulted in the excessive wear of their teeth. The normal drifting of the teeth to compensate for this wear ensured that space was available for most wisdom teeth to erupt by adolescence. However, our modern diet is softer, so wear is minimal so drift is also minimal, resulting in less space for wisdom teeth to erupt naturally. Why remove them? If a wisdom tooth doesn’t have room to grow (impacted wisdom tooth), this may result in pain, infection or other dental problems. The patient will then probably need to have it removed. The extraction of wisdom teeth is generally necessary when they are prevented from properly erupting within the mouth. Poor alignment of wisdom teeth can crowd or damage adjacent teeth, the jawbone, and nerves. Wisdom teeth that lean toward the second molars make those teeth more vulnerable to decay by entrapping plaque and debris. This can lead to swollen and sore gums (pericoronitis), tooth decay, jaw stiffness and infection. Partially erupted teeth are also more prone to tooth decay and gum disease because their hard-to-reach location and awkward positioning makes brushing and flossing difficult. Other issues that can arise include the formation of tumours or cysts around the impacted tooth. This can in turn result in permanent damage to the jawbone and other, healthy teeth. What happens next? Dr Ehlers will exam and take an X-Ray of your mouth. This will allow him to see the extent of the impaction or eruption and to plan a course of action suitable to your particular case. Depending on his assessment Dr Ehlers will advise you on whether it is better to have a procedure where local anaesthetic (you will be awake during the procedure) is used or general anaesthetic (you will be asleep during the procedure). During a local anaesthetic procedure your gum area will be numbed around the wisdom tooth/teeth, so you will feel no pain. In addition, Dr Ehlers may opt to use a sedative which will help you to relax during the procedure. During the procedure, the tooth may be cut into smaller parts to make it easier to remove through the opening. There’s less need to make an incision if the tooth has already erupted through the gum. Should you need to be admitted to hospital as a day patient, you will be given a general anaesthetic which will make you sleep. Read more about after-procedure care
Removal of impacted teeth Surgical removal of all wisdom teeth and impacted teeth. An impacted tooth is a tooth that is unable to erupt into its normal position in the jaw. This is usually caused by the tooth becoming blocked in-between two adjacent teeth or by the tooth being formed in an abnormal position. The most commonly affected teeth are the wisdom teeth/third molars and the canines. Wisdom teeth are the last teeth to erupt in your mouth, usually between the ages of 17 and 25. In ancient times, the rough diet people followed resulted in the excessive wear of their teeth. The normal drifting of the teeth to compensate for this wear ensured that space was available for most wisdom teeth to erupt by adolescence. However, our modern diet is softer, so wear is minimal so drift is also minimal, resulting in less space for wisdom teeth to erupt naturally. Why remove them? If a wisdom tooth doesn’t have room to grow (impacted wisdom tooth), this may result in pain, infection or other dental problems. The patient will then probably need to have it removed. The extraction of wisdom teeth is generally necessary when they are prevented from properly erupting within the mouth. Poor alignment of wisdom teeth can crowd or damage adjacent teeth, the jawbone, and nerves. Wisdom teeth that lean toward the second molars make those teeth more vulnerable to decay by entrapping plaque and debris. This can lead to swollen and sore gums (pericoronitis), tooth decay, jaw stiffness and infection. Partially erupted teeth are also more prone to tooth decay and gum disease because their hard-to-reach location and awkward positioning makes brushing and flossing difficult. Other issues that can arise include the formation of tumours or cysts around the impacted tooth. This can in turn result in permanent damage to the jawbone and other, healthy teeth. What happens next? Dr Ehlers will exam and take an X-Ray of your mouth. This will allow him to see the extent of the impaction or eruption and to plan a course of action suitable to your particular case. Depending on his assessment Dr Ehlers will advise you on whether it is better to have a procedure where local anaesthetic (you will be awake during the procedure) is used or general anaesthetic (you will be asleep during the procedure). During a local anaesthetic procedure your gum area will be numbed around the wisdom tooth/teeth, so you will feel no pain. In addition, Dr Ehlers may opt to use a sedative which will help you to relax during the procedure. During the procedure, the tooth may be cut into smaller parts to make it easier to remove through the opening. There’s less need to make an incision if the tooth has already erupted through the gum. Should you need to be admitted to hospital as a day patient, you will be given a general anaesthetic which will make you sleep. Read more about after-procedure care  Dental implantology Dr Ehlers is involved in the planning, placement, and exposure of dental implants; immediate implant placement after extraction as well as Customised guides and stents. What is a dental implant? Absent teeth can be replaced by placing titanium implants in the jaw in the area of the absent teeth. A crown or bridge will then be placed on the dental implant. While dental implants may need periodic adjustments, they can last a lifetime when properly placed and cared for over time. A face without teeth can sag and appear sunken and sad. Dental implants allow you to maintain the natural shape of your face and smile. Leaving empty spaces in your mouth after losing one or more teeth can lead to additional health issues, such as the loss and deterioration of some of your jawbone. When it is not being used to support a natural tooth, the jawbone deteriorates, losing its strength and firmness. Dental implants are the only dental restoration option that preserves and stimulates natural bone, actually helping to stimulate bone growth and prevent bone loss. Cavities can’t occur in an implant-restored crown, or replacement tooth; however, you will need to visit your dentist as scheduled and clean and care for it and your gums and mouth every day, the same as you would if it were a natural tooth. It is advised that you have an implant done as soon as possible after having an extraction to ensure bone integrity.
Dental implantology Dr Ehlers is involved in the planning, placement, and exposure of dental implants; immediate implant placement after extraction as well as Customised guides and stents. What is a dental implant? Absent teeth can be replaced by placing titanium implants in the jaw in the area of the absent teeth. A crown or bridge will then be placed on the dental implant. While dental implants may need periodic adjustments, they can last a lifetime when properly placed and cared for over time. A face without teeth can sag and appear sunken and sad. Dental implants allow you to maintain the natural shape of your face and smile. Leaving empty spaces in your mouth after losing one or more teeth can lead to additional health issues, such as the loss and deterioration of some of your jawbone. When it is not being used to support a natural tooth, the jawbone deteriorates, losing its strength and firmness. Dental implants are the only dental restoration option that preserves and stimulates natural bone, actually helping to stimulate bone growth and prevent bone loss. Cavities can’t occur in an implant-restored crown, or replacement tooth; however, you will need to visit your dentist as scheduled and clean and care for it and your gums and mouth every day, the same as you would if it were a natural tooth. It is advised that you have an implant done as soon as possible after having an extraction to ensure bone integrity. 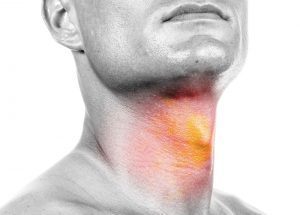 Management of head and neck infections Emergency treatment of all head and neck infections. A tooth abscess is a pocket of pus that’s caused by a bacterial infection. The abscess can occur at different regions of the tooth for different reasons. A periapical abscess occurs at the tip of the root. The most common source of infections in the head and neck area is a tooth abscess. A periapical tooth abscess occurs when bacteria invade the dental pulp — the innermost part of the tooth that contains blood vessels, nerves and connective tissue. Bacteria enter through either a dental cavity or a chip or crack in the tooth and spread all the way down to the root. The bacterial infection can cause swelling and inflammation at the tip of the root. Leaving a tooth abscess untreated can lead to serious, even life-threatening, complications. Symptoms may include:
Management of head and neck infections Emergency treatment of all head and neck infections. A tooth abscess is a pocket of pus that’s caused by a bacterial infection. The abscess can occur at different regions of the tooth for different reasons. A periapical abscess occurs at the tip of the root. The most common source of infections in the head and neck area is a tooth abscess. A periapical tooth abscess occurs when bacteria invade the dental pulp — the innermost part of the tooth that contains blood vessels, nerves and connective tissue. Bacteria enter through either a dental cavity or a chip or crack in the tooth and spread all the way down to the root. The bacterial infection can cause swelling and inflammation at the tip of the root. Leaving a tooth abscess untreated can lead to serious, even life-threatening, complications. Symptoms may include:
- Severe, persistent, throbbing toothache that can radiate to the jawbone, neck or ear
- Sensitivity to hot and cold temperatures
- Sensitivity to the pressure of chewing or biting
- Fever
- Swelling in your face or cheek
- Tender, swollen lymph nodes under your jaw or in your neck
- Sudden rush of foul-smelling and foul-tasting, salty fluid in your mouth and pain relief if the abscess ruptures.
Do not ignore the important signs of pain and fever, as they usually indicate the likelihood of a significant infection. In many cases, the symptoms can be treated with antibiotics and warm saltwater rinses. However, in serious cases, the abscess may need to be lanced (incised) and drained. It is important that one seeks medical help at the first signs of an abscess to prevent the condition becoming more serious. In extreme cases a small infection can spread down the throat, and can even travel to the chest cavity. Where the upper teeth are affected, the infection usually spreads to the cheek and the area under the eye. Some of the veins in this area do not have valves, so blood can flow backward and in extremely severe cases, spread infection to an area under the brain, known as the cavernous sinus. 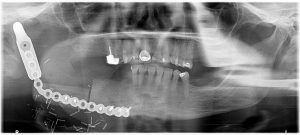 Facial reconstruction surgery Defects in the jaw and or facial bones are reconstructed using the patient’s own tissue and/or artificial materials. What are defects in the jaw and facial bone and how does one treat them? Patients may develop jaw defects for a number of reasons. An injury due to facial trauma or infection can cause damage to the jaw bone. Defects may also be a result of flawed developmental processes. For some reasons, the jaw may not develop fully in certain regions, leading to jaw defects. Some pathologic processes involving the jaw bone such cysts, tumours, or head and neck cancers can lead to jaw deformities. A jaw defect can affect your ability to chew, speak, or even breathe properly, and it can also have a negative impact on your appearance and your self-esteem. Surgical interventions can help correct jaw defects, restore the patient aesthetically, and give the patient the ability to chew and function properly. Bone grafting can repair implant sites with inadequate bone structure due to previous extractions, gum disease or injuries. The bone is either obtained from a tissue bank or your own bone is taken from the jaw, hip or fibula (below the knee.) Sinus bone grafts are also performed to replace bone in the posterior upper jaw. In addition, special membranes may be utilised that dissolve under the gum and protect the bone graft and encourage bone regeneration. This is called guided bone regeneration or guided tissue regeneration. Major bone grafts are typically performed to repair defects of the jaws. These defects may arise as a result of traumatic injuries, tumour surgery, or congenital defects. Large defects are repaired using the patient’s own bone. This bone is harvested from a number of different sites depending on the size of the defect. The skull (cranium), hip (iliac crest), and lateral knee (fibula), are common donor sites. These procedures are routinely performed in an operating room and require a hospital stay. Orthognathic surgery usually involves a realignment of the existing jaw structure while reconstructive surgery usually connotes the rebuilding or replacement of missing jaw structure.
Facial reconstruction surgery Defects in the jaw and or facial bones are reconstructed using the patient’s own tissue and/or artificial materials. What are defects in the jaw and facial bone and how does one treat them? Patients may develop jaw defects for a number of reasons. An injury due to facial trauma or infection can cause damage to the jaw bone. Defects may also be a result of flawed developmental processes. For some reasons, the jaw may not develop fully in certain regions, leading to jaw defects. Some pathologic processes involving the jaw bone such cysts, tumours, or head and neck cancers can lead to jaw deformities. A jaw defect can affect your ability to chew, speak, or even breathe properly, and it can also have a negative impact on your appearance and your self-esteem. Surgical interventions can help correct jaw defects, restore the patient aesthetically, and give the patient the ability to chew and function properly. Bone grafting can repair implant sites with inadequate bone structure due to previous extractions, gum disease or injuries. The bone is either obtained from a tissue bank or your own bone is taken from the jaw, hip or fibula (below the knee.) Sinus bone grafts are also performed to replace bone in the posterior upper jaw. In addition, special membranes may be utilised that dissolve under the gum and protect the bone graft and encourage bone regeneration. This is called guided bone regeneration or guided tissue regeneration. Major bone grafts are typically performed to repair defects of the jaws. These defects may arise as a result of traumatic injuries, tumour surgery, or congenital defects. Large defects are repaired using the patient’s own bone. This bone is harvested from a number of different sites depending on the size of the defect. The skull (cranium), hip (iliac crest), and lateral knee (fibula), are common donor sites. These procedures are routinely performed in an operating room and require a hospital stay. Orthognathic surgery usually involves a realignment of the existing jaw structure while reconstructive surgery usually connotes the rebuilding or replacement of missing jaw structure.  Dentoalveolar surgery Dentoalveolar surgery includes all surgical procedures that involves the teeth and surrounding tissue such as dental extractions, surgical removal of teeth, exposure of unerupted teeth, bone contouring, apicectomies (remove the tip/apex of the root of a tooth), etc. Common problems requiring dentoalveolar surgery:
Dentoalveolar surgery Dentoalveolar surgery includes all surgical procedures that involves the teeth and surrounding tissue such as dental extractions, surgical removal of teeth, exposure of unerupted teeth, bone contouring, apicectomies (remove the tip/apex of the root of a tooth), etc. Common problems requiring dentoalveolar surgery:
- Trauma or decay. All attempts will be made to fix a damaged or decayed tooth but in some cases extraction will be necessary.
- Crowded teeth. A tooth may need to be pulled to allow for the proper alignment of the other teeth.
- When tooth decay or tooth damage spreads into the tooth’s pulp — the sensitive centre of the tooth that holds nerves and blood vessels — bacteria can get into the pulp and cause infection. It’s possible that damage and infection can be remedied through root canal therapy. When a root canal and antibiotics don’t resolve the infection, tooth extraction may be necessary to stop the infection from getting worse and spreading.
- Compromised immune system. Sometimes a tooth needs to be extracted if there’s a chance that it may become infected. This is the case if a patient has a compromised immune system, such as during chemotherapy or after an organ transplant.
- Gum disease. Periodontal disease, commonly known as gum disease, is one of the leading causes of tooth loss. The bone and connective tissue that keeps the teeth in place start to break down from bacterial toxins and the body’s natural immune response to the infection. If left untreated, the bones, gums, and tissue that support the teeth are destroyed. The teeth become loose over time and require extraction.
Procedures can range from simple extractions to extremely complex procedures and often a combination of procedures requiring extraction, modification to the bone, and/or modification of the gum tissue surrounding the surgical site. Dentoalveolar procedures may include a combination of the following:
- Partial or full tooth extraction
- Removal of bone material
- Reshaping of bone material
- Soft tissue removal
- Soft tissue repair.
How a tooth is extracted With the help of x-rays, your oral surgeon will determine the best way to remove the tooth or teeth. There are two types of extractions:
- Simple extraction.
If the tooth is visible in the mouth, Dr Ehlers will use a tool called an elevator to loosen the tooth and then removes the tooth with forceps, under local anaesthetic.
- Surgical extraction.
This more complicated procedure is necessary when a tooth is below the gum line, whether the tooth has broken that far down, or it hasn’t come in yet. This usually requires a small incision in the gum. It may also call for removing some bone or cutting a tooth in half in order to take the tooth out. You’ll receive a local anaesthetic for a surgical extraction, and you may also receive general anesthesia. Read more here for after-procedure mouth and tooth care 
Treatment of facial trauma Treatment of facial bone fractures as well as injuries to the soft tissue of the face. Facial trauma can be severe. Among its major causes are auto accidents, sports injuries, work-related mishaps, falls, and acts of violence. When serious facial injury occurs, it’s important that you receive immediate and comprehensive care. Facial trauma in general involves injuries to the soft- or hard-tissue structures of the face, mouth or jaws — including the teeth, the bones of the jaws and face, and the tissue of the skin and gums. It can also involve treatment of particular specialised regions, such as the area around the eyes, the salivary glands or facial nerves. Because facial injuries can affect not only a person’s ability to carry on basic life functions (eating, vision, etc.) but also his or her appearance, there is often a strong emotional component to treatment as well as a physical one. Some facial traumas are relatively minor. A common one occurs when a tooth is loosened or knocked out (avulsed). Many times, if treated immediately, Dr Ehlers can successfully re-implant the tooth in the jaw. If that isn’t possible, placing a dental implant is often the most effective way to replace a missing tooth. Another type of relatively common but more serious injury may involve a fracture of the facial bones, including the cheekbones, upper or lower jawbones, or the eye sockets. In principle, the treatment is essentially the same as that used for a broken arm: place the bones back in their proper position, and immobilise them. But since it isn’t possible to put a cast on the face, different immobilisation techniques are used. One method involves wiring the upper and lower jaws together to let them heal in the correct alignment; alternatively, plates and screws may be used to permanently reattach the bones. Severe facial trauma is often a critical condition, since over 60% of these patients also have serious injuries in other parts of the body. In fact, many of the standard techniques used in trauma centres were developed by oral and maxillofacial surgeons during the wars in Korea, Vietnam, and the Middle East. Restoring breathing, controlling bleeding and checking for neurological damage are top priorities. After that, Dr Ehlers will attempt to accomplish as much of the reconstructive surgery as possible in one operation.
 Benign and malignant head and neck tumours Diagnosis and surgical removal of tumours of the jaw, facial soft tissue and intra-oral tumours. Oral cancer’s mortality rate is particularly high, not because it is hard to detect or diagnose, but because the cancer is often discovered late in its development. Your family dentist or Dr Ehlers is in the best position to detect oral cancer during your routine dental examinations. A staggering 90% of head and neck cancers are squamous cell carcinomas (HNSCC). HNSCC is the sixth leading cancer by incidence worldwide. HNSCC are not gender, age or race specific, hence anyone can develop it. The five-year survival rate of patients with HNSCC is about 40-50%. Head and neck cancers often spread to the lymph nodes of the neck, and this is often the first (and sometimes only) sign of the disease at the time of diagnosis. It is suggested that you perform an oral cancer self-examination monthly. Do this using a bright light and a mirror:
Benign and malignant head and neck tumours Diagnosis and surgical removal of tumours of the jaw, facial soft tissue and intra-oral tumours. Oral cancer’s mortality rate is particularly high, not because it is hard to detect or diagnose, but because the cancer is often discovered late in its development. Your family dentist or Dr Ehlers is in the best position to detect oral cancer during your routine dental examinations. A staggering 90% of head and neck cancers are squamous cell carcinomas (HNSCC). HNSCC is the sixth leading cancer by incidence worldwide. HNSCC are not gender, age or race specific, hence anyone can develop it. The five-year survival rate of patients with HNSCC is about 40-50%. Head and neck cancers often spread to the lymph nodes of the neck, and this is often the first (and sometimes only) sign of the disease at the time of diagnosis. It is suggested that you perform an oral cancer self-examination monthly. Do this using a bright light and a mirror:
- Remove any dentures
- Look and feel inside the lips and the front of gums
- Tilt head back to inspect and feel the roof of your mouth
- Pull the cheek out to see its inside surface as well as the back of the gums
- Pull out your tongue and look at all of its surfaces
- Feel for lumps or enlarged lymph nodes (glands) in both sides of the neck including under the lower jaw.
Your mouth is one of your body’s most important early warning systems. Don’t ignore any suspicious lumps or sores. Should you discover something, make an appointment for a prompt examination. Early treatment may well be the key to complete recovery. Other symptoms of head and neck cancer include:
- Enlarged lymph node
- Sore throat
- Hoarse voice.
- Bleeding from the mouth
- Nasal congestion, especially with nasopharyngeal carcinoma
- Bad breath
- Sore tongue
- Painless ulcer or sores in the mouth that do not heal
- White, red or dark patches in the mouth that will not go away
- Earache
- Numbness
- Lump in the lip, mouth or gums.
While these may well be symptoms of something less sinister than cancer, if they persist, one should definitely investigate further. Dr Ehlers will perform a biopsy to determine a diagnosis. These may be followed by a CT-scan, MRI-scan, PET-scan and blood tests. In cooperation with oncologists and a reconstructive surgical team, Dr Ehlers will devise a treatment plan which will possibly entail surgery.  Orthognathic surgery Corrective jaw surgery to position the jaws into their correct relationship and to correct misalignment of jaws and teeth. Corrective jaw, or orthognathic surgery is performed by an oral and maxillofacial surgeon (OMS) to correct a wide range of minor and major skeletal and dental irregularities, including the misalignment of jaws and teeth. Surgery can improve chewing, speaking and breathing. While the patient’s appearance may be dramatically enhanced as a result of their surgery, orthognathic surgery is primarily performed to correct functional problems. Some of the conditions that may indicate the need for corrective jaw surgery:
Orthognathic surgery Corrective jaw surgery to position the jaws into their correct relationship and to correct misalignment of jaws and teeth. Corrective jaw, or orthognathic surgery is performed by an oral and maxillofacial surgeon (OMS) to correct a wide range of minor and major skeletal and dental irregularities, including the misalignment of jaws and teeth. Surgery can improve chewing, speaking and breathing. While the patient’s appearance may be dramatically enhanced as a result of their surgery, orthognathic surgery is primarily performed to correct functional problems. Some of the conditions that may indicate the need for corrective jaw surgery:
- Difficulty chewing or biting food
- Difficulty swallowing
- Chronic jaw or jaw joint (TMJ) pain and headache
- Excessive wear of the teeth
- Open bite (space between the upper and lower teeth when the mouth is closed)
- Unbalanced facial appearance from the front, or side
- Facial injury
- Birth defects
- Receding lower jaw and chin
- Protruding jaw
- Inability to make the lips meet without straining
- Chronic mouth breathing
- Sleep apnoea (breathing problems when sleeping, including snoring).
The procedure used in Orthognathic surgery is known as Mandibular Osteotomy. The operation is undertaken through an incision made at the back of the mouth in the gum by the molar teeth to gain access to the jaw. The lower jaw is then cut in an oblique fashion with a small saw to allow it to be broken in a controlled manner. It is then moved into its new position, which has been predetermined during surgical planning with the aid of models of your teeth. A small plastic wafer is attached to the teeth to allow the new position of the lower jaw to be determined, which is then fixed into place with small metal plates and screws. These are made of titanium that is a very inert metal and safe to be used in the body. The gum is stitched back into place with dissolvable stitches.  TMJ disorders and facial pain Diagnosis and treatment of all TMJ (temporomandibular joint) pain, including joint rinsing, abnormal joint sounds and functional joint problems. The temporomandibular joint (TMJ) acts like a sliding hinge, connecting your jawbone to your skull. You have one joint on each side of your jaw. TMJ disorders — a type of temporomandibular disorder or TMD — can cause pain in your jaw joint and in the muscles that control jaw movement. The exact cause of a person’s TMJ disorder is often difficult to determine. Your pain may be due to a combination of factors, such as genetics, arthritis or jaw injury. Some people who have jaw pain also tend to clench or grind their teeth, although many people habitually clench or grind their teeth and never develop TMJ disorders. Signs and symptoms of TMJ disorders may include:
TMJ disorders and facial pain Diagnosis and treatment of all TMJ (temporomandibular joint) pain, including joint rinsing, abnormal joint sounds and functional joint problems. The temporomandibular joint (TMJ) acts like a sliding hinge, connecting your jawbone to your skull. You have one joint on each side of your jaw. TMJ disorders — a type of temporomandibular disorder or TMD — can cause pain in your jaw joint and in the muscles that control jaw movement. The exact cause of a person’s TMJ disorder is often difficult to determine. Your pain may be due to a combination of factors, such as genetics, arthritis or jaw injury. Some people who have jaw pain also tend to clench or grind their teeth, although many people habitually clench or grind their teeth and never develop TMJ disorders. Signs and symptoms of TMJ disorders may include:
- Pain or tenderness of your jaw
- Pain in one or both of the temporomandibular joints
- Aching pain in and around your ear
- Difficulty chewing or pain while chewing
- Aching facial pain
- Locking of the joint, making it difficult to open or close your mouth.
TMJ disorders can also cause a clicking sound or grating sensation (with associated pain) when you open your mouth or chew. If other treatment methods don’t help, you may need surgery which includes:
- Arthrocentesis. Arthrocentesis (ahr-throe-sen-TEE-sis) is a minimally invasive procedure that involves the insertion of small needles into the joint so that fluid can be irrigated through the joint to remove debris and inflammatory byproducts.
- Injections. In some people, corticosteroid injections into the joint may be helpful. Infrequently, injecting botulinum toxin type A (Botox, others) into the jaw muscles used for chewing may relieve pain associated with TMJ disorders.
- TMJ arthroscopy. In some cases, arthroscopic surgery can be as effective for treating various types of TMJ disorders as open-joint surgery. A small thin tube (cannula) is placed into the joint space, an arthroscope is then inserted, and small surgical instruments are used for surgery. TMJ arthroscopy has fewer risks and complications than open-joint surgery does, but it has some limitations as well.
- Modified condylotomy. This addresses the TMJ indirectly, with surgery on the mandible, but not in the joint itself. It may be helpful for treatment of pain and if locking is experienced.
- Open-joint surgery. If your jaw pain does not resolve with more-conservative treatments and it appears to be caused by a structural problem in the joint, open-joint surgery (arthrotomy) to repair or replace the joint may be suggested. However, open-joint surgery involves more risks than other procedures do and should be considered very carefully, discussing the pros and cons.
 Management of facial pain Diagnosis, work-up and management of facial pain and neuralgias. Recurring episodes of severe pain along your face could mean you have trigeminal neuralgia (TN). Although not always curable, TN can be managed effectively with the right strategy. TN affects a specific pair of nerves called the trigeminal that signal pain in the face or jaws. They originate from the brain stem through the skull on either side of the face, with each nerve having upper, middle and lower branches. TN can affect one or more of these branches and cause anywhere from a mild twinge to excruciating pain. Causes for TN differ in individual patients. Though it could be linked to a tumour, lesion or cold sore, it most often seems to arise from a blood vessel impinging on the nerve and damaging its outer coating. This causes it to be hypersensitive: chewing, speaking or even lightly touching the face can set it off. The damaged nerve may also fail to ‘shut off’ when the triggering stimulation stops. If you have these types of symptoms, your first step is to obtain an accurate diagnosis. You’ll need a thorough examination to rule out other possibilities like jaw joint problems or a tooth abscess. Once it has been confirmed that it’s definitely TN, Dr Ehlers can then devise a treatment strategy. Treatment will usually begin with conservative measures like medication to block pain transmission to the brain or anticonvulsants that stabilise the nerve and decrease abnormal firing. If medication isn’t enough, an invasive procedure may be considered to control symptoms. One such surgical solution is known as percutaneous treatment in a thin needle is insert to selectively damage nerve fibres to prevent their firing. If it’s determined that an artery or vein has compressed the nerve, the vessel might be surgically relocated. These techniques can be quite effective but they do have possible side effects like numbness or hearing loss.
Management of facial pain Diagnosis, work-up and management of facial pain and neuralgias. Recurring episodes of severe pain along your face could mean you have trigeminal neuralgia (TN). Although not always curable, TN can be managed effectively with the right strategy. TN affects a specific pair of nerves called the trigeminal that signal pain in the face or jaws. They originate from the brain stem through the skull on either side of the face, with each nerve having upper, middle and lower branches. TN can affect one or more of these branches and cause anywhere from a mild twinge to excruciating pain. Causes for TN differ in individual patients. Though it could be linked to a tumour, lesion or cold sore, it most often seems to arise from a blood vessel impinging on the nerve and damaging its outer coating. This causes it to be hypersensitive: chewing, speaking or even lightly touching the face can set it off. The damaged nerve may also fail to ‘shut off’ when the triggering stimulation stops. If you have these types of symptoms, your first step is to obtain an accurate diagnosis. You’ll need a thorough examination to rule out other possibilities like jaw joint problems or a tooth abscess. Once it has been confirmed that it’s definitely TN, Dr Ehlers can then devise a treatment strategy. Treatment will usually begin with conservative measures like medication to block pain transmission to the brain or anticonvulsants that stabilise the nerve and decrease abnormal firing. If medication isn’t enough, an invasive procedure may be considered to control symptoms. One such surgical solution is known as percutaneous treatment in a thin needle is insert to selectively damage nerve fibres to prevent their firing. If it’s determined that an artery or vein has compressed the nerve, the vessel might be surgically relocated. These techniques can be quite effective but they do have possible side effects like numbness or hearing loss.
